Explaining non-adherence – The Capability, Opportunity, Motivation, and Behavior (COM-B) framework
- There are many reasons, some modifiable, that patients do not adhere to cardiovascular-disease treatments, therefore, a comprehensive framework for assessing and understanding adherence is needed1
- The COM-B system is a framework for understanding behavior that has been applied to adherence, encompassing Capability, Opportunity and Motivation2,3
- COM-B allows for a precise understanding of the relationship between the individual and adherence, making it easier to identify appropriate interventions for patients2
There is a need for a comprehensive framework for assessing adherence
Systematic reviews of non-adherence indicate that there are a myriad of reasons why patients may not adhere to their treatment regimens.1
These include both modifiable reasons that can be targeted for change, such as patient knowledge and understanding of their disease, the support available to them, and non- modifiable causes, such as age and gender.1
A review of 51 systematic reviews covering 19 different disease categories and assessing non- adherence to chronic therapies identified over 750 individual factor items. The vast majority of these were related to treatment implementation, with a small proportion linked to persistence.1
| Term | Definition |
| Treatment implementation1 | How well a patient’s dosing corresponds to the prescribed dosing regimen |
| Persistence1 | The length of time between starting the medicine and taking the final dose before discontinuation |
In cardiovascular disease specifically, reasons for non-adherence vary. Studies have suggested that medicines may be commonly discontinued due to side effects, confusion over the prescription, cost or mistrust of the therapy or health care system.4 Other linked factors include psychosocial issues, such as depression.5 Further evidence shows that medication non-adherence may vary depending on other external factors; medication non-adherence may be relatively low initially following a cardiovascular event, but usually increases over time.6
Taken together, these issues suggest that multifaceted interventions may be the most effective way to address unsatisfactory adherence, one such example may be practical social support from friends and family.7
COM-B is a new approach to classifying causes of non-adherence
The COM-B system is a framework for understanding behavior.3
The factors which influence health-related behaviors can be placed into three broad groups:2,3
| Capability | ‘The physical or psychological ability to engage in the activity concerned’, e.g. a patient with heart disease may find it difficult to swallow their medication, or struggle to remember to take it |
| Opportunity | ‘All the factors that lie outside the individual that make the behavior possible, or prompt it’, e.g. the patient may be unable to access appropriate healthcare due to its cost |
| Motivation | ‘Brain processes that energize and direct behavior’, e.g. a patient with hypertension may not feel they need to take treatment and are worried about side effects |
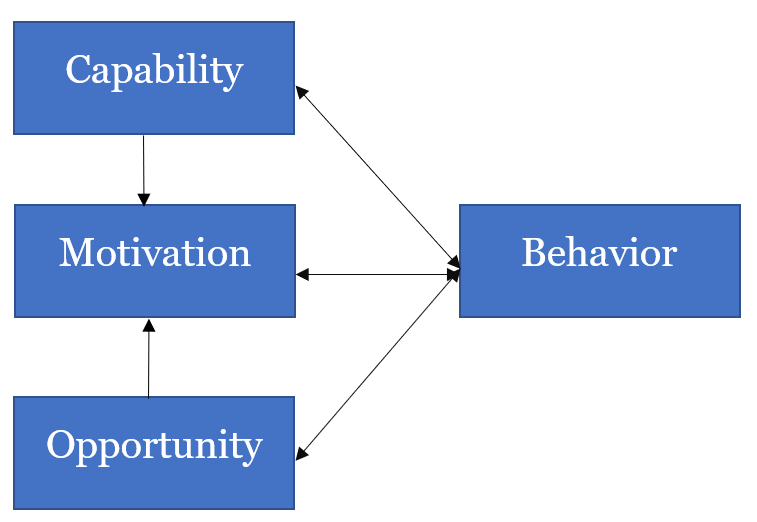
The model hypothesizes that the interaction between these three components causes behavior. Each can impact behavior directly; and, in addition, Opportunity and Capability might influence Motivation and so affect behavior. The COM-B framework is a dynamic model – performance of a behavior can in turn influence Capability, Opportunity and Motivation.2
This general framework has now been applied to adherence. It is intended as a starting point in order to choose interventions that are mostly likely to be effective in clinical practice.2
Capability
The definition of capability is the individual’s ability, both psychological and physical, to engage in the activity concerned, including possessing the necessary knowledge and skills to do so.3
Psychological factors in relation to adherence include comprehension of disease and treatment, cognitive thinking (e.g. memory, capacity for judgement, thinking) and executive function (e.g. the capacity to plan).2
Physical capabilities are important in allowing patients to adapt to lifestyle changes (e.g. diet or social behaviors). Dexterity, or the ability to swallow, may also be important in allowing patients to take their medications appropriately.2
Opportunity
Opportunity is defined as all the factors that make the behavior possible, or prompt it. These can be divided into physical and social categories.2
‘Physical’ relates to the physical opportunity provided by the environment. This encompasses factors such as cost, access to medication, physical characteristics of the medicine (e.g. taste, smell, size, shape, route of administration), and regimen complexity.2
Social opportunity factors include social support and the relationship/standard of communication between the physician and the patient.2
Motivation
Motivation broadly covers all brain processes that energize and direct behavior. Within the COM-B framework, motivational factors can be described as ‘Reflective’ or ‘Automatic’.2
Reflective motivations cover evaluations and plans. For adherence, this would include the patient’s perception of their illness (e.g. its cause, timeline [i.e. chronic vs acute], consequences etc.), their beliefs about the treatment (e.g. its necessity, efficacy, any concerns about current or future adverse events, and any general aversion to taking medicines), their expectancies about outcome of treatment, and their belief in their own capabilities in sticking to treatment.2
Automatic motivations are emotions and impulses that arise from associative learning and/or innate dispositions. These would cover stimuli or cues for action, as well as mood states or any mood disorders that the patient may be living with, such as depression or anxiety.2
Advantages of COM-B in understanding adherence
COM-B has various advantages in explaining adherence compared with the narrower models that preceded it. It includes automatic processes such as habit, unlike social cognition models that have previously been applied to adherence. COM-B’s specificity also allows a precise description of the relationship between the characteristics of the patient and their adherence, making it easier to identify appropriate interventions.2













